Understanding Healthcare's Environmental Footprint and the Path to Sustainable Medicine
- Dr. Satishchandra Chauhan
- 38 minutes ago
- 7 min read

Environmental sustainability is not merely an ecological concern—it is a public health imperative. Edwin Chadwick recognized this connection as early as 1842, when he documented the direct relationship between environmental conditions and human health outcomes. Nearly two centuries later, that relationship is more consequential than ever. Clean air, safe water, uncontaminated soil, and a stable climate are not luxuries; they are prerequisites for human health.
Herein lies a profound irony: the healthcare sector—whose stated purpose is to protect and restore health—is itself a significant contributor to the environmental conditions that threaten it. Healthcare is responsible for an estimated 5–10% of global carbon dioxide emissions. For clinicians and health system leaders, this duality presents both a moral challenge and a professional responsibility.
The Carbon Cost of Clinical Care
Healthcare is a resource-intensive system. Every clinical interaction—from a primary care consultation to a complex surgical procedure—carries a measurable carbon footprint spanning energy use, consumable production, transport logistics, and waste disposal.
The emissions generated are more significant than many in the sector appreciate:
A routine dental appointment generates approximately 17.9 kg of CO₂ equivalent emissions
A single surgical operation produces between 100 and 300 kg of CO₂ equivalent—comparable to driving a petrol car 400–1,200 km
The MedTech sector alone accounted for 4.4% of total global emissions of 37.12 billion tonnes of CO₂e recorded in April 2023
Clinical Illustration: A large urban hospital performing 15 elective laparoscopic cholecystectomies per day generates approximately 1,500–4,500 kg of CO₂ equivalent from surgical activity alone. This excludes pre-operative investigations, post-operative inpatient stay, pharmaceutical use, and patient transport. Over a year, surgical emissions from a single busy operating suite can rival those of a mid-sized manufacturing facility—yet this dimension of hospital operations rarely features in institutional sustainability reporting.

Beyond the Hospital: Pharmaceutical and Medical Device Pollution
The environmental burden of healthcare extends well beyond hospital walls. Two sectors merit particular attention from clinicians and administrators:
The Pharmaceutical Industry
Drug manufacturing is energy- and water-intensive, with significant chemical waste generated at every stage of synthesis. Beyond production, medicinal residues—active pharmaceutical ingredients (APIs) that pass through patients and enter wastewater systems—present a growing ecological threat. Studies have detected antimicrobials, hormones, and cytotoxic agents in rivers, groundwater, and even drinking water sources globally.
Clinical Illustration: A 2019 study published in Science of the Total Environment detected measurable concentrations of the antibiotic ciprofloxacin downstream from pharmaceutical manufacturing sites in Hyderabad, India, at levels sufficient to drive antimicrobial resistance in environmental bacteria. The ecological and public health implications extend far beyond the individual patient for whom the drug was prescribed. This underscores why clinicians' prescribing choices carry an environmental dimension alongside a clinical one.
The Medical Device and MedTech Sector
Medical devices generate greenhouse gas emissions across their entire lifecycle—from raw material extraction and manufacturing, through distribution and clinical use, to disposal. Many devices—including imaging equipment, ventilators, and surgical instruments—rely on rare earth elements and complex supply chains spanning multiple continents. Life-saving technology and environmental responsibility are not inherently in conflict, but realizing their compatibility requires intentional design and procurement decisions.
Conducting full life-cycle assessments (LCA) of pharmaceutical products and medical devices—evaluating environmental impact from synthesis to disposal—represents one of the most rigorous and actionable steps health systems can take to understand and reduce their ecological footprint.
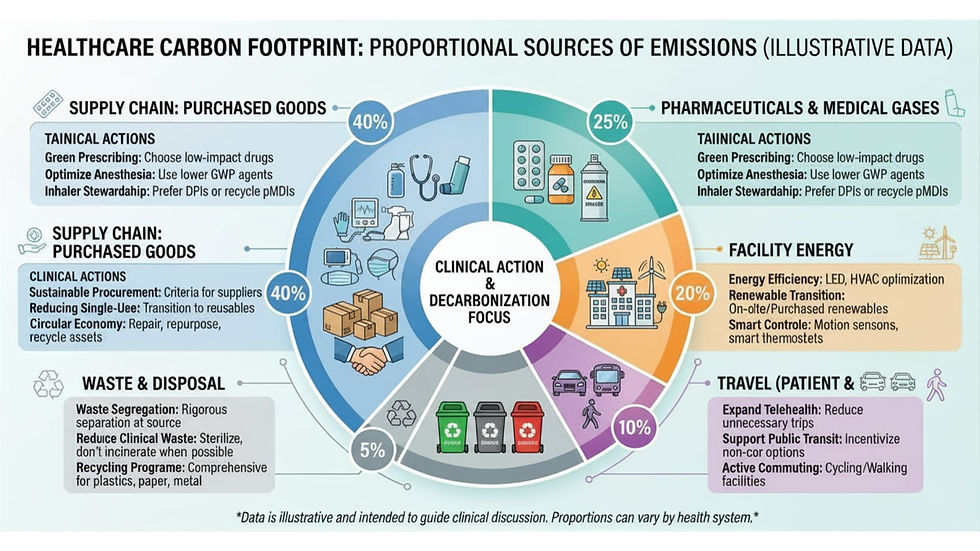
Key Sources of Healthcare's Environmental Footprint
A systematic understanding of where healthcare emissions originate is essential for prioritizing interventions:
Infrastructure and construction: hospital building and maintenance consume significant natural resources and contribute to urban heat islands
Energy use: hospitals are among the most energy-intensive buildings in any country, relying heavily on fossil fuels for HVAC, lighting, sterilization, and life-support systems
Patient and staff transport: indirect emissions from commuting, patient transfers, and medical supply logistics form a substantial share of total healthcare emissions
Chemical and pharmaceutical waste: solvent emissions, disinfectants, sterilizing agents, and improper disposal of hazardous chemicals contaminate both air and water
Radiation: medical imaging technologies, including CT scanners and fluoroscopy equipment, contribute to environmental radiation exposure
Healthcare waste: plastics, sharps, infectious materials, and expired pharmaceuticals remain poorly managed in many health systems
Hospital wastewater: effluents carrying pathogens, drug residues, and chemical contaminants are frequently discharged into water systems without adequate treatment
Why the Transition to Green Healthcare Is Slow: Structural Barriers
Identifying the sources of healthcare pollution is the relatively straightforward part. Designing and implementing viable alternatives is considerably more complex. Several structural barriers impede progress:
Green Chemistry in pharmaceutical manufacturing can substantially reduce hazardous waste, but its adoption remains limited due to weak regulatory mandates and economic disincentives for existing producers
Replacing single-use disposables presents genuine clinical dilemmas — infection control protocols, particularly in operating theatres and intensive care units, were largely designed around single-use equipment, and reusable alternatives require robust sterilisation pathways
Inconsistent emission benchmarking: the absence of standardised global guidelines for healthcare carbon measurement prevents meaningful cross-institutional comparison and collective accountability
Medical device sustainability involves complex trade-offs between performance, cost, material availability, and patient safety compliance — constraints that slow the uptake of eco-designed alternatives
Medical plastic recycling remains technically challenging due to contamination risk, mixed polymer composition, and insufficient regulatory frameworks in most countries
Financial disincentives: high upfront costs of green infrastructure, combined with limited short-term ROI, discourage investment in sustainability among resource-constrained institutions
Clinical Illustration: A regional hospital attempted to transition its operating theatres from single-use draping systems to reusable textile alternatives. While the environmental case was clear, the initiative stalled due to concerns from the infection control team about laundering standards, a lack of approved vendor supply, and a 40% higher upfront procurement cost despite a projected 5-year cost saving. This exemplifies how patient safety concerns, when not proactively addressed with evidence, can become barriers to sustainability transitions.
Practical Pathways to Sustainable Healthcare Delivery
The transition to sustainable healthcare does not require the dismantling of existing systems. Many of the most impactful interventions are refinements of established practice, now supported by modern technology:
1. Frugal Innovation in Medical Device Design
Devices designed around essential functionality, using locally sourced materials, reduce both material consumption and distribution-related emissions. The GE MAC 400 portable ECG machine—designed for use in rural India—is a widely cited example: it delivers core diagnostic capability at a fraction of the energy, cost, and material use of conventional ECG systems, and has since been adopted in resource-limited settings globally.
2. Green Building Design and Energy Management
Hospitals designed or retrofitted to maximise natural light, cross-ventilation, and passive cooling substantially reduce dependence on fossil-fuel-powered HVAC systems. AI-driven energy management platforms have demonstrated the capacity to reduce hospital energy consumption by 30–50% compared to conventional systems, while simultaneously improving the reliability and consistency of environmental conditions in clinical areas.
Clinical Illustration: Indira Gandhi Memorial Hospital in the Maldives—a tropical climate with high cooling demands—implemented an AI-integrated building management system that optimised real-time HVAC load distribution based on patient occupancy. Within 18 months, electricity consumption fell by 34%, equivalent to a reduction of approximately 600 tonnes of CO₂ annually. Critically, internal clinical environment standards were maintained throughout.
3. Reusable and Biodegradable Medical Supplies
Where infection control evidence supports it, substituting single-use plastics with reusable or biodegradable alternatives can significantly reduce both waste volume and procurement costs. Programmes at NHS trusts in the United Kingdom that switched to reusable surgical gowns and instrument trays demonstrated 20–30% reductions in plastic waste from operating theatres without adverse infection outcomes.
4. Preventive Healthcare and Climate-Resilient Communities
Every hospitalisation averted through effective preventive care is also an emission averted. Integrating climate health literacy into community medicine programmes—educating populations about heat-related illness, vector-borne disease risk, food and water safety under changing climate patterns—builds health system resilience at the community level, reducing reactive, high-emission emergency care demand.
Clinical Illustration: During the extreme heat events of summer 2022 across South Asia, community health workers in several districts of Rajasthan proactively identified vulnerable populations—elderly individuals with cardiovascular disease, outdoor labourers, and infants—and delivered targeted hydration and shade guidance. In the districts where this programme operated, heat-related hospital admissions were 28% lower than in comparator districts. Preventive action delivered measurable clinical and environmental benefit simultaneously.
5. Sustainable Anaesthetic Practice
Volatile anaesthetic agents are among the most potent greenhouse gases used in medicine. Desflurane, for example, has a global warming potential approximately 2,500 times that of CO₂. Transitioning to total intravenous anaesthesia (TIVA) or to lower-impact agents such as sevoflurane, and implementing anaesthetic gas capture systems, represents a high-impact, clinician-driven sustainability intervention that requires no change to infrastructure.

The Clinician's Role in Planetary Health
Healthcare professionals are uniquely positioned to drive the sustainability transition—not merely as institutional administrators, but as clinicians whose daily decisions carry environmental consequences. Prescribing habits, choice of anesthetic agent, investigation ordering patterns, single-use versus reusable equipment preferences, and end-of-life medication advice are all clinical decisions with environmental dimensions.
Clinician-led sustainability encompasses:
Rational prescribing — minimizing unnecessary antimicrobials, single-dose over multi-dose vials where appropriate, and avoiding over-prescription of pharmaceuticals with known environmental persistence
Advocating for green formulary policies at the institutional and national level
Integrating environmental outcome measures alongside clinical outcomes in quality improvement initiatives
Participating in or leading hospital sustainability committees
Educating junior colleagues and medical students on planetary health as a core clinical competency
Medical associations and postgraduate training bodies are increasingly embedding planetary health into curricula. The expectation that clinicians understand the environmental impact of their practice is becoming a standard of professional competence, not a peripheral interest.

Conclusion: Sustainable Healthcare as a Professional Imperative
The United Nations' definition of sustainable development—meeting the needs of the present without compromising the ability of future generations to meet theirs—is not an abstract policy aspiration. It is a clinical mandate. Every patient we treat today lives in the environment that our collective choices are shaping.
The barriers to sustainable healthcare—economic, technical, and regulatory—are real but not insurmountable. What is required is coordinated commitment: strategic policy from governments, investment from hospital leadership, evidence-based action from clinicians, and accountability across supply chains. Fragmented awareness without structural action will be insufficient.
Embracing sustainability does not compromise clinical excellence—it advances it. Health systems that reduce their environmental footprint also tend to be more efficient, more resilient, and more equitable. The imperative to heal and the imperative to protect the environment are not in tension. They are, ultimately, the same imperative.
Key Takeaways for Healthcare Professionals
Healthcare contributes 5–10% of global CO₂ emissions — clinicians are part of both the problem and the solution.
A single surgical procedure can generate 100–300 kg of CO₂ equivalent — equivalent to driving a car hundreds of kilometers.
Pharmaceutical residues in water systems drive antimicrobial resistance and ecological harm — rational prescribing is an environmental act.
The MedTech sector alone accounted for 4.4% of global CO₂e emissions in 2023 — device lifecycle thinking matters.
AI-driven energy management can reduce hospital energy consumption by 30–50% without compromising clinical standards.
Sustainable anesthesia — switching from desflurane to TIVA or sevoflurane — is a high-impact, zero-infrastructure-cost intervention.
Preventive healthcare is low-carbon healthcare — every hospitalization averted is an emission averted.
Sustainability and clinical excellence are complementary, not competing, goals.




Comments